Applications of Machine Learning in retinal diseases

Artificial Intelligence and related terms (Machine Learning, Deep Learning, etc.) have received a lot of attention in recent years in the media, and yet the precise understanding of these words remains elusive to the general audience. Artificial Intelligence is the field of computer science devoted to the development of machines whose abilities are typically associated to human functions, such as learning. Machine Learning, in turn, is the field of Artificial Intelligence dedicated to the development of statistical models and algorithms to make that happen, while another commonly used term, Deep Learning, a subset of Machine Learning, does so based on artificial neural networks, methods that emulate how human brains think (Figure). In Ophthalmology there has been an increasing use of both, Machine Learning and Deep Learning, in recent years.
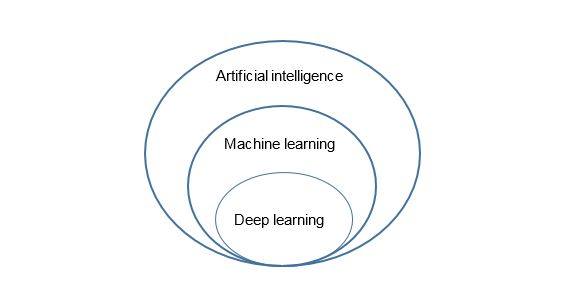
Figure. Relationship between Artificial intelligence, Machine Learning and Deep learning.
There are two approaches to Machine Learning. In the supervised approach, the ophthalmologist annotates the features of interest (fluid, drusen) in images (retina scan or optical coherence tomography [OCT], for example) or databases, and an algorithm is developed to learn the relationship between the image and the labelling by the specialist, which requires many (thousands) of images or data. In other words, it learns by example, and the final goal is prediction. In unsupervised Machine Learning, the data (images, for example) are not labelled and the overall aim is to develop a statistical model that describes the findings de novo. This may uncover a priori unknown relationships, and the final goal is an improved understanding of the data.
On the other hand, Deep Learning in ophthalmology is mostly focused on image analysis. It has been shown that Deep Learning-based systems have been able to detect diabetic retinopathy, age-related macular degeneration or retinopathy or prematurity 1 on fundus photographs with a level of accuracy similar to that of human graders. In another study,2 the algorithm even identified the age, sex, blood pressure and smoking status from fundus photography alone. Other imaging modalities, notably OCT, are also amenable to Deep Learning applications for automatic detection and quantification of retinal fluid 3 and even for referral decisions. 4 In fact, the Food and Drug Administration (FDA), the organism in charge of granting approval of drugs and medical devices in the US) recently approved the first Deep Learning-based software that detected signs of “referable” (more than mild) diabetic retinopathy.5
In summary, the potential of Artificial intelligence-based methods is enormous. It spans aspects related to screening, diagnosis, treatment, prediction (response to treatment) and even disclosure of previously unknown relationships. It will be regularly used in the care of patients with retinal disorders in the years to come.
References
- Ting DSW et al. Deep learning in ophthalmology: The technical and clinical considerations. Prog Retin Eye Res; in press.
- Poplin R et al. Prediction of cardiovascular risk factors from retinal fundus photographs via deep learning. Nat Biomed Eng 2018; 2: 158-64.
- Schmidt-Erfürth U et al. Artificial intelligence in retina. Prog Retin Eye Res 2018; 67: 1-29.
- De Fauw J et al. Clinically applicable Deep learning for diagnosis and referral in retinal disease. Nat Med 2018; 24: 1342-50.
- Verbraak FD et al. Diagnostic accuracy of a device for the automated detection of diabetic retinopathy in a primary care setting. Diab Care 2019; 42: 651-6.
Author: Marc Biarnés OD MPH PhD, member of the BMF research team